9 0 5 7 8
论文已发表
注册即可获取德孚的最新动态
IF 收录期刊
- 2.6 Breast Cancer (Dove Med Press)
- 3.9 Clin Epidemiol
- 3.3 Cancer Manag Res
- 3.9 Infect Drug Resist
- 3.6 Clin Interv Aging
- 4.8 Drug Des Dev Ther
- 2.8 Int J Chronic Obstr
- 8.0 Int J Nanomed
- 2.3 Int J Women's Health
- 3.2 Neuropsych Dis Treat
- 4.0 OncoTargets Ther
- 2.2 Patient Prefer Adher
- 2.8 Ther Clin Risk Manag
- 2.7 J Pain Res
- 3.3 Diabet Metab Synd Ob
- 4.3 Psychol Res Behav Ma
- 3.4 Nat Sci Sleep
- 1.9 Pharmgenomics Pers Med
- 3.5 Risk Manag Healthc Policy
- 4.5 J Inflamm Res
- 2.3 Int J Gen Med
- 4.1 J Hepatocell Carcinoma
- 3.2 J Asthma Allergy
- 2.3 Clin Cosmet Investig Dermatol
- 3.3 J Multidiscip Healthc

术后肝动脉灌注化疗提高了胰腺癌根治术后胰腺癌的存活率:一项回顾性研究
Authors Wang Y, Xu Y, Zheng Y, Bao Y, Wang P
Received 12 October 2017
Accepted for publication 5 January 2018
Published 21 February 2018 Volume 2018:11 Pages 903—907
DOI https://doi.org/10.2147/OTT.S153886
Checked for plagiarism Yes
Review by Single-blind
Peer reviewers approved by Dr Amy Norman
Peer reviewer comments 2
Editor who approved publication: Dr Tohru Yamada
Objective: To determine the effect of postoperative hepatic arterial infusion
chemotherapy (HAIC) on long-term survival of patients with pancreatic cancer
(PC) after radical pancreatectomy.
Methods: A total of 87 patients with PC underwent radical
pancreatectomy in the First People’s Hospital affiliated to Huzhou Normal
College between June 2008 and May 2013. Among these patients, after surgery, 43
received two sessions of HAIC followed by four sessions of systemic
chemotherapy (HAIC group), while 44 received six sessions of systemic
chemotherapy alone (control group). Both the HAIC and systemic chemotherapy
regimen included 5-fluorouracil (1,000 mg/m2) as a 5-h
infusion on day 1, and gemcitabine (800 mg/m2) as an over
30-min infusion on days 1 and 8. The toxicity, complication, and long-term
survival were retrospectively compared.
Results: No significant difference in patient
characteristics between the two groups was found. No chemotherapy-related
deaths were recorded, and no significant difference in toxicities was observed
between the two groups. The 5-year disease-free survival probability did not
differ between the two groups (P =0.2029, hazard
ratio for recurrence=0.7561; 95% CI=0.4768–1.1989, by the log-rank test). The
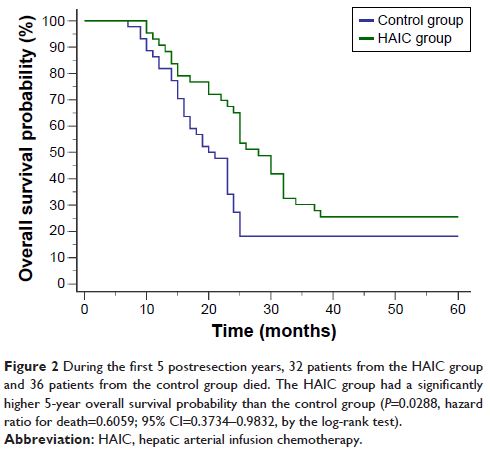
HAIC group had significantly higher 5-year overall survival probability (P =0.0288, hazard ratio for
death=0.6059; 95% CI=0.3734–0.9832, by the log-rank test) and higher 5-year
hepatic metastases-free survival probability (P =0.0321,
hazard ratio for hepatic metastases=0.5006; 95% CI=0.2546–0.9843, by the
log-rank test) than the control group.
Conclusions: Postoperative HAIC has the potential to prevent
hepatic metastases and increase long-term survival probability of patients with
PC after radical pancreatectomy.
Keywords: pancreatic
cancer, hepatic arterial infusion chemotherapy, hepatic metastases, survival