9 0 6 7 6
论文已发表
注册即可获取德孚的最新动态
IF 收录期刊
- 2.6 Breast Cancer (Dove Med Press)
- 3.9 Clin Epidemiol
- 3.3 Cancer Manag Res
- 3.9 Infect Drug Resist
- 3.6 Clin Interv Aging
- 4.8 Drug Des Dev Ther
- 2.8 Int J Chronic Obstr
- 8.0 Int J Nanomed
- 2.3 Int J Women's Health
- 3.2 Neuropsych Dis Treat
- 4.0 OncoTargets Ther
- 2.2 Patient Prefer Adher
- 2.8 Ther Clin Risk Manag
- 2.7 J Pain Res
- 3.3 Diabet Metab Synd Ob
- 4.3 Psychol Res Behav Ma
- 3.4 Nat Sci Sleep
- 1.9 Pharmgenomics Pers Med
- 3.5 Risk Manag Healthc Policy
- 4.5 J Inflamm Res
- 2.3 Int J Gen Med
- 4.1 J Hepatocell Carcinoma
- 3.2 J Asthma Allergy
- 2.3 Clin Cosmet Investig Dermatol
- 3.3 J Multidiscip Healthc

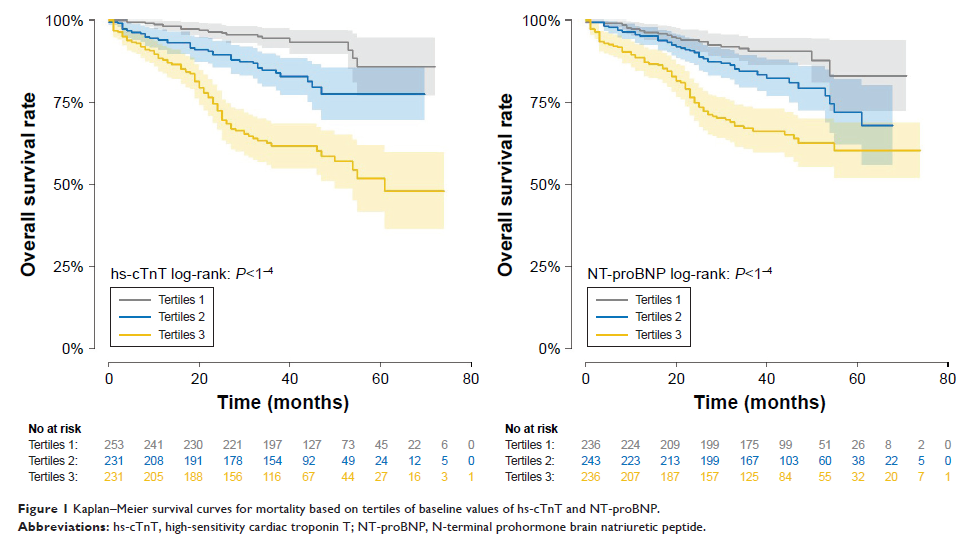
高敏感性心肌肌钙蛋白 T 和 N 末端激素原脑利钠肽的预后值之间的对比,以评估老年住院患者的死亡率
Authors Chen JR, Wang Q, Wu W, Zhang SJ
Received 16 September 2018
Accepted for publication 3 December 2018
Published 31 December 2018 Volume 2019:14 Pages 81—90
DOI https://doi.org/10.2147/CIA.S187757
Checked for plagiarism Yes
Review by Single-blind
Peer reviewers approved by Dr Andrew Yee
Peer reviewer comments 3
Editor who approved publication: Dr Zhi-Ying Wu
Background: Studies
have shown that increases in low-level high-sensitivity cardiac troponin T
(hs-cTnT) and N-terminal prohormone brain natriuretic peptide (NT-proBNP) in
the elderly population lead to high risk of adverse clinical outcomes, such as
mortality. In this study, associations between the two biomarkers and long-term
mortality in elderly patients hospitalized for medical conditions other than
acute cardiovascular events were investigated. A comparison of the predictive
value of hs-cTnT and NT-proBNP for all-cause mortality was conducted.
Methods: A cohort
of 715 elderly inpatients free of acute cardiovascular events was initially
recruited. Based on tertiles of baseline hs-cTnT and NT-proBNP levels, the
elderly were arranged into low, middle, and high groups. The mortality of each
group was observed and the predictive values of hs-cTnT and NT-proBNP compared.
Additionally, all-cause mortality was analyzed for hs-cTnT and NT-proBNP
combined.
Results: There
were 135 (18.9%) all-cause mortality cases identified during follow-up (median
47 months). The upper tertile of hs-cTnT was significantly associated with an
increased risk of mortality (HR 3.29, 95% CI 1.85–5.85), even after adjustment
for potential confounders. However, there were no significant differences
observed in mortality rates among the three NT-proBNP groups after adjustment for
potential confounders (HR 1.77, 95% CI 0.83–3.17). Compared to NT-proBNP,
hs-cTnT was a better predictor of mortality, as area under curves for hs-cTnT
and NT-proBNP at 60 months were 0.712 (95% CI 0.616–0.809) and 0.585 (95% CI
0.483–0.6871), respectively. Also, the combination of the two cardiac
biomarkers did not render a better predictive value for mortality than hs-cTnT
alone.
Conclusion: Unlike
hs-cTnT, baseline NT-proBNP levels failed to show an independent association
with all-cause mortality in hospitalized elderly without acute cardiovascular
events. hs-cTnT provided significant prognostic value for mortality in the
study cohort.
Keywords: high-sensitivity
cardiac troponin T (hs-cTnT), N-terminal prohormone brain natriuretic peptide
(NT-proBNP), nonacute cardiovascular events, elderly patients