9 0 5 7 8
论文已发表
注册即可获取德孚的最新动态
IF 收录期刊
- 2.6 Breast Cancer (Dove Med Press)
- 3.9 Clin Epidemiol
- 3.3 Cancer Manag Res
- 3.9 Infect Drug Resist
- 3.6 Clin Interv Aging
- 4.8 Drug Des Dev Ther
- 2.8 Int J Chronic Obstr
- 8.0 Int J Nanomed
- 2.3 Int J Women's Health
- 3.2 Neuropsych Dis Treat
- 4.0 OncoTargets Ther
- 2.2 Patient Prefer Adher
- 2.8 Ther Clin Risk Manag
- 2.7 J Pain Res
- 3.3 Diabet Metab Synd Ob
- 4.3 Psychol Res Behav Ma
- 3.4 Nat Sci Sleep
- 1.9 Pharmgenomics Pers Med
- 3.5 Risk Manag Healthc Policy
- 4.5 J Inflamm Res
- 2.3 Int J Gen Med
- 4.1 J Hepatocell Carcinoma
- 3.2 J Asthma Allergy
- 2.3 Clin Cosmet Investig Dermatol
- 3.3 J Multidiscip Healthc

曲伏前列素与噻吗洛尔治疗玻璃体切除术后早期发作的眼压升高的疗效和安全性:一项随机试验
Authors Fang Y, Ku H, Gan D, Jiang R, Sun X
Received 11 July 2019
Accepted for publication 18 September 2019
Published 30 September 2019 Volume 2019:13 Pages 3453—3463
DOI https://doi.org/10.2147/DDDT.S222796
Checked for plagiarism Yes
Review by Single-blind
Peer reviewers approved by Dr Melinda Thomas
Peer reviewer comments 2
Editor who approved publication: Professor Jianbo Sun
Purpose: To evaluate the efficacy and safety of travoprost 0.004% versus timolol 0.5% as an initial intraocular pressure (IOP)-lowering medication for ocular hypertension secondary to vitrectomy.
Patients and methods: We performed a randomized, controlled, observer-blinded clinical trial in the Eye & ENT Hospital of Fudan University in China. This trial was registered at www.chictr.org.cn (ChICTR1800014942) before patient enrollment. Seventy-nine adults with IOP of 25–45 mmHg secondary to vitrectomy in the latest one month were enrolled and randomized to receive travoprost 0.004% or timolol 0.5%. More drugs were administered to patients with IOP > 25 mmHg during follow-up.
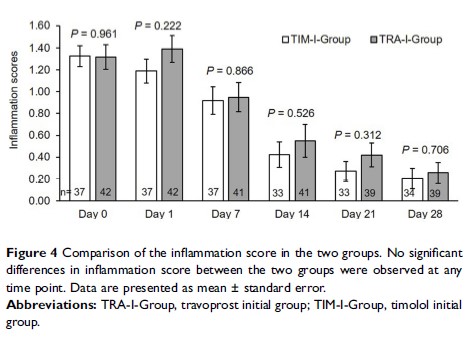
Results: The mean IOP reduction at day 1 was −10.97 mmHg in the timolol group and −15.02 mmHg in the travoprost group (P = 0.006); no significant difference was observed between the groups at later time points. The number of IOP-lowering medications at day 21 was 0.64 in the timolol group and 1.15 in the travoprost group (P = 0.038), while no significant differences were observed at other time points. The proportion of single IOP-lowering medications used during the 4-week follow-up was 72.73% in the timolol group and 68.42% in the travoprost group (P = 0.692). Inflammation scores were not significantly different in the two groups at any time point. Increased ocular hyperemia occurred in 8 patients (19%) in the travoprost group and none in the timolol group (P = 0.005). There were no significant differences in other adverse events between the two groups. After logistic regression model analysis, IOP ≥ 30 mmHg, inflammation score ≥ 2, and silicone oil as tamponade were found to be the factors with significant effects on the number of IOP-lowering medications used during the 4-week follow-up.
Conclusion: Travoprost and timolol have similar efficacy and safety for treating ocular hypertension secondary to vitrectomy.
Keywords: travoprost, timolol, vitrectomy, ocular hypertension, early-onset